CONTACT
We will reply as soon as possible.
Enevia Health, LLC
30 N Gould Ste N, Sheridan, WY 82801, USA
Font: https://neurosciencenews.com/microglia-alzheimers-genetics-25230/
A new study by researchers at MIT's Picower Institute for Learning and Memory details how the mutation undermines microglia function, explaining how it appears to lead to that increased risk.
"This TREM2 R47H/+ mutation is a pretty strong risk factor for Alzheimer's disease," said the study's lead author, Jay Penney, a former postdoc in the MIT lab of Picower Professor Li-Huei Tsai. Penney is now an incoming assistant professor at the University of Prince Edward Island
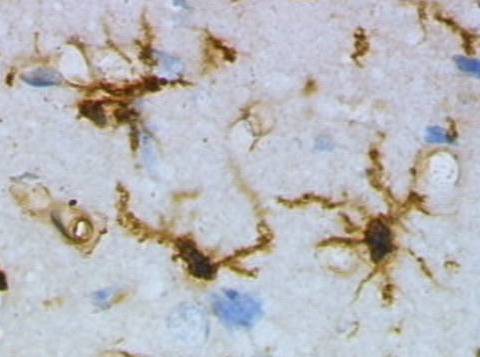
"This study adds clear evidence that microglia dysfunction contributes to the risk of Alzheimer's disease."
In the study published in the journal GLIA, Tsai and Penney's team shows that human microglia with the R47H/+ mutation in the TREM2 protein present several deficits related to Alzheimer's pathology. Mutant microglia are prone to inflammation, but respond less well to neuronal injury and are less able to remove harmful waste, including the amyloid beta protein characteristic of Alzheimer's.
When scientists transferred TREM2 mutant human microglia into the brains of mice, the mice suffered a significant decrease in the number of synapses, or connections between their neurons, which may disrupt circuits that enable brain functions such as memory.
This study is not the first to ask that question, but it may advance scientists' emerging understanding, Penney said. Early studies suggested that the mutation simply stripped the protein of its function, but new evidence paints a deeper and more nuanced picture.
While microglia show reduced waste clearance and response to injury, they become hyperactive in other ways, such as excessive inflammation and synapse pruning.
"There is a partial loss of function but also a gain of function for certain things," Penney said.
Instead of relying on mouse models with the TREM2 R47H/+ mutation, Penney, Tsai and their co-authors focused their work on cultures of human microglia cells. To do this, they used a line of stem cells derived from skin cells donated by a healthy 75-year-old woman.
Then, in some of the stem cells they used CRISPR gene editing to insert the R47H/+ mutation and then grew edited and unedited stem cells to turn them into microglia. This strategy provided them with a supply of mutated microglia and healthy microglia, to act as experimental controls, who were otherwise genetically identical.
The team then examined how harboring the mutation affected the expression of its genes in each cell line. The scientists measured more than 1,000 differences, but one especially notable finding was that microglia with the mutation increased the expression of genes associated with inflammation and immune responses.

Then, when they exposed microglia in culture to chemicals that mimic infection, the mutant microglia demonstrated a significantly more pronounced response than normal microglia, suggesting that the mutation makes microglia much more prone to inflammation.
In additional experiments with the cells, the team exposed them to three types of debris that microglia normally remove in the brain: myelin, synaptic proteins, and amyloid beta. The mutant microglia cleared less than the healthy ones.
Another function of microglia is to respond when cells, such as neurons, are injured. Penney and Tsai's team grew microglia and neurons and then bombarded them with a laser.
For the next 90 minutes after injury, the team tracked the movement of surrounding microglia. Compared to normal microglia, those with the mutation were less likely to home in on the injured cell.
Finally, to test how mutant microglia act in a living brain, the scientists transplanted healthy or mutant control microglia into mice into a memory-focused region of the brain called the hippocampus. The scientists then stained that region to highlight several proteins of interest.
Having normal or mutant human microglia didn't matter for some measures, but proteins associated with synapses were significantly reduced in mice implanted with the mutated microglia.
By combining evidence from gene expression measurements and evidence from microglial function experiments, the researchers were able to formulate new ideas about what drives at least some of the microglial misbehavior.
For example, Penney and Tsai's team noted a decrease in the expression of a "purinergic" receptor protein involved in detecting neuronal injury, which perhaps explains why the mutant microglia had difficulty with that task.
They also observed that mice with the mutation overexpressed "complementary" proteins used to mark synapses for elimination. That could explain why the mutant microglia were overzealous about eliminating synapses in the mice, Penney said, although increased inflammation could also cause that by damaging neurons in general.
As the molecular mechanisms underlying microglial dysfunction become clearer, Penney said, drug developers will gain critical insights into ways to address the increased disease risk associated with the TREM2 R47H/+ mutation.
"Our findings highlight multiple effects of the TREM2 R47H/+ mutation that likely underlie its association with Alzheimer's disease risk and suggest new nodes that could be exploited for therapeutic intervention," the authors conclude.
These discoveries highlight the complexity of neurological diseases and highlight the importance of continued research.
Visit our other articles on our blog through: https://eneviahealth.com/blog/ and remember that at Enevia we care about your health!
We will reply as soon as possible.
30 N Gould Ste N, Sheridan, WY 82801, USA
Our groups are the ideal platform to learn and share your scientific concerns about neurodevelopment issues
*Our purpose is informational only, it is not intended to be a substitute for medical advice, diagnosis or treatment.
We are working on our website. For any queries, you can contact our customer service team at atencionalcliente@eneviahealth.com